In high-stakes surgeries such as brain tumor removal, precision can mean the difference between recovery and irreversible damage. The CUSA machine (Cavitron Ultrasonic Surgical Aspirator) is a breakthrough tool that uses ultrasonic energy to remove diseased tissue while safeguarding vital nerves and blood vessels. Renowned for its unmatched tissue selectivity, this technology has redefined possibilities in neurosurgery, liver surgery, and other complex procedures. This guide explores how the CUSA machine works, its uses, benefits, and the innovations shaping its future.
Table of Contents
The Science Behind the Scalpel: How a CUSA Machine Works
To understand the CUSA machine’s impact, one must first appreciate that it is not a cutting tool in the traditional sense of a scalpel or scissors. It doesn’t slice or tear. Instead, it employs low-frequency ultrasound energy to selectively fragment, liquefy, and aspirate targeted tissue. This section will demystify the sophisticated physics and engineering that make this possible.
The Core Principle: Ultrasonic Tissue Ablation
The magic of the CUSA machine lies in a process called ultrasonic tissue ablation, which is a symphony of three simultaneous actions: fragmentation, irrigation, and aspiration.
- Fragmentation & Emulsification: The handpiece’s surgical tip vibrates at 23–36 kHz, breaking cellular bonds like a microscopic jackhammer. It also triggers cavitation—microscopic bubbles that collapse with force—further breaking down soft tissue into a liquefied slurry.
- Tissue Selectivity: This is the CUSA machine’s most celebrated feature. Its selectivity comes from tissue composition. Structures rich in collagen and elastin—like blood vessels, nerves, and organ capsules—are resilient enough to withstand ultrasonic vibrations without fragmenting. This lets surgeons “shave away” soft tumors from delicate arteries or nerves while keeping them intact. Tissues with weak bonds and high fluid content fragment easily, while those with strong bonds resist fragmentation (SAGES).
- Irrigation and Aspiration: These functions work alongside fragmentation. A constant stream of sterile saline cools the tip to prevent thermal damage and helps emulsify tissue. At the same time, an integrated suction system removes the emulsified tissue and fluid through the tip’s hollow center, keeping the surgical field clean and the anatomy clearly visible.
Anatomy of a CUSA System
A complete CUSA system is composed of several interconnected components, each playing a vital role in its function.
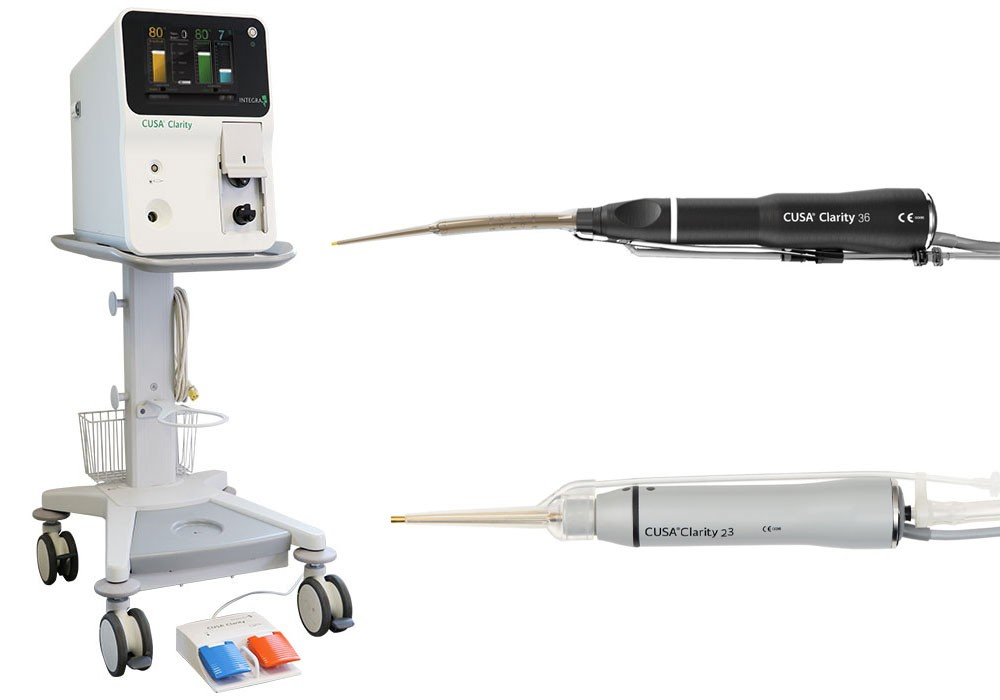
The Integra CUSA Clarity system, showing the console with its display, two distinct handpieces (23 kHz and 36 kHz), and the foot pedal for surgical control
- The Console: The “brain” of the system, it’s a mobile cart containing the ultrasonic generator, electronics, and pumps for irrigation and suction. From its control panel or touchscreen, surgeons or staff can adjust settings like vibration amplitude, suction level, and irrigation flow to suit the tissue being resected (Skill Biomed).
- The Handpiece: This is the instrument the surgeon holds. It is a marvel of engineering, containing a transducer that converts the electrical energy supplied by the console into high-frequency mechanical vibrations. There are two primary types of transducers used:
- Magnetostrictive: This type uses a coil to generate a magnetic field, which causes a stack of nickel alloy plates within the handpiece to rapidly expand and contract (oscillate), producing the vibration (AIIMSNET).
- Piezoelectric: This more modern type uses special ceramic crystals that physically change shape when a voltage is applied, generating a very efficient and precise vibration (PI Ceramic White Paper).
- Magnetostrictive: This type uses a coil to generate a magnetic field, which causes a stack of nickel alloy plates within the handpiece to rapidly expand and contract (oscillate), producing the vibration (AIIMSNET).
- The Surgical Tip: The “business end” of the device, it makes contact with tissue and is interchangeable for versatility. Available in various lengths, diameters, and shapes, each tip is designed for specific procedures and tissue types—for example, a robust tip for removing a tough tumor and a fine tip for precision work near a cranial nerve (PMC4279210).
- Accessories: The system is completed by a range of accessories, including foot pedals that allow for hands-free control of the device, sterile single-use tubing sets for irrigation and aspiration, and maintenance kits to ensure the longevity and performance of the reusable handpieces.
Precision in Practice: Key Clinical Applications of the CUSA Machine
The unique properties of the CUSA machine—namely its tissue selectivity and ability to maintain a clear surgical field—make it an indispensable tool in surgeries where precision and the preservation of vital structures are not just beneficial, but absolutely paramount. Its use has become standard practice in some of the most challenging surgical specialties.
Neurosurgery: The Brain and Spine
Nowhere is precision more critical than in the brain and spinal cord. The CUSA machine has been a cornerstone of modern neurosurgery for decades, first cleared by the FDA for this use as early as 1980 under product code “LBK” (FDA Executive Summary, 2022).
- Core Application: Tumor Resection: The CUSA machine is widely used to remove intracranial tumors such as gliomas, meningiomas, and metastases (PubMed). Its main advantage is internal debulking—surgeons can reduce a tumor’s mass from the inside out, making it safer and easier to separate from surrounding healthy brain tissue.
- Specific Scenarios:
- Skull Base Surgery: This is perhaps the CUSA’s most valued application. It allows surgeons to remove tumors from anatomically treacherous locations where critical cranial nerves and major arteries, like the internal carotid artery, are encased by or intimately associated with the tumor.
- Spinal Cord Tumors: The device enables the safe removal of tumors located within or adjacent to the delicate spinal cord, minimizing the risk of postoperative neurological deficits.
- Skull Base Surgery: This is perhaps the CUSA’s most valued application. It allows surgeons to remove tumors from anatomically treacherous locations where critical cranial nerves and major arteries, like the internal carotid artery, are encased by or intimately associated with the tumor.
- Benefit Highlight: The paramount benefit in neurosurgery is the preservation of critical neural and vascular structures. This directly translates to better patient outcomes, preserving functions like vision, movement, and sensation that would otherwise be at high risk.
Hepatobiliary (Liver) Surgery
The liver’s anatomy makes it an ideal candidate for CUSA machine use. Its soft, water-rich parenchyma can be fragmented easily with ultrasound, while the tougher, fibrous blood vessels and bile ducts remain preserved.
- Core Application: Liver Resection (Hepatectomy): The CUSA is used to perform precise anatomical resections, carefully dissecting the liver parenchyma along specific planes.
- Specific Scenarios: As the CUSA removes the liver cells, it leaves the network of blood vessels and bile ducts intact and exposed, like a skeletonized tree. The surgeon can then clearly identify, ligate (tie off), and divide these structures under direct vision.
- Benefit Highlight: This technique significantly reduces two of the major risks in liver surgery: intraoperative blood loss and postoperative bile leakage. Studies have shown that ultrasonic devices can lead to better outcomes in hepatectomy compared to traditional methods (World Journal of Surgical Oncology).
Other Expanding Applications
While neurosurgery and liver surgery remain its primary domains, the utility of the CUSA machine is being recognized across a growing number of specialties:
- Gynecology: For the resection of large uterine fibroids or complex cases of endometriosis (Fertility and Sterility).
- Urology: In partial nephrectomy, where a tumor is removed from a kidney while preserving the rest of the organ.
- Ophthalmology: For delicate procedures in the confined space of the orbit, such as bony orbital decompression in thyroid eye disease or the removal of orbital tumors (IJCEO).
- Cardiac Surgery: In complex cases requiring decalcification of the mitral or aortic annulus, where the CUSA can precisely remove calcium deposits without damaging surrounding valve structures (MMCTS).
Case Spotlight: Resecting a Skull Base Meningioma with CUSA
To truly appreciate the CUSA’s impact, consider a real-world scenario based on published case reports.
Patient Profile: A 46-year-old patient presents with headaches and decreasing vision. An MRI reveals a large, tough sphenoid ridge meningioma—a benign but challenging tumor—located at the base of the skull. The tumor is compressing the optic nerve and has encased the internal carotid artery, the main blood supply to that side of the brain.
Surgical Challenge: The goal is total tumor removal to decompress the optic nerve and prevent further vision loss. However, achieving this without causing permanent blindness or a catastrophic, life-threatening bleed from the carotid artery is a formidable challenge.
CUSA in Action: The neurosurgeon employs the CUSA Excel system. They begin by setting the device to a high power setting to debulk the dense, fibrous center of the tumor, quickly reducing its volume. As they approach the critical structures, they adjust the parameters, lowering the power and increasing the “Tissue Select” function. With meticulous care, the surgeon uses the vibrating tip to fragment the tumor tissue layer by layer, literally peeling it away from the delicate surfaces of the optic nerve and the carotid artery. The CUSA’s tissue selectivity is the key enabling factor, allowing the resilient nerve and artery to remain unharmed while the tumor emulsifies and is suctioned away.
Outcome: As documented in a study from Shanghai Huashan Hospital, this technique allows for the complete resection of the tumor. Post-operative imaging confirms no residual tumor, and most importantly, the critical neurovascular structures are preserved. The patient recovers well, with their vision stabilized or improved, a testament to the precision afforded by the CUSA machine (Application of CUSA Excel, PMC).
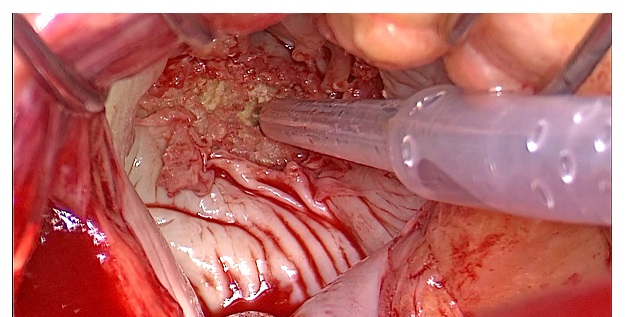
Intraoperative view showing a CUSA probe selectively removing tissue while preserving adjacent vascular structures, highlighting the device’s precision
CUSA vs. The Field: A Comparative Look at Surgical Technologies
While the CUSA machine is a powerful instrument, it is one of several advanced energy devices available to surgeons. Understanding its unique strengths and weaknesses in comparison to other common tools is crucial for selecting the right instrument for the right job. Each technology has a distinct mechanism and is best suited for different tasks.
| Technology | Working Principle | Best For | Key Advantage | Key Limitation |
|---|---|---|---|---|
| CUSA | Ultrasonic fragmentation, emulsification, and aspiration. | Soft, high-water-content tissue (tumors, liver parenchyma); debulking. | Unmatched tissue selectivity; spares vessels/nerves. Keeps field clear. | Limited hemostasis (coagulation); potential for thermal injury without proper irrigation. |
| Harmonic Scalpel | High-frequency ultrasonic vibration of a blade to cut and coagulate simultaneously. | Dissection and hemostasis in one step; transecting vascularized tissue. | Excellent hemostasis (seals vessels up to 7mm); less thermal spread than electrosurgery. | Less tissue-selective than CUSA; creates a smoke plume. |
| Water Jet (WJ) Dissector | A high-pressure, fine jet of saline dissects tissue by separating planes. | Parenchymal transection, especially in liver surgery. | Athermal (no heat damage); excellent exposure of vascular/biliary structures. | Provides no hemostasis; requires a separate coagulation device. Can obscure the field. |
| Electrosurgery (Bovie) | High-frequency electrical current passes through tissue to cut or coagulate. | General-purpose cutting and coagulation; widely available and versatile. | Fast and effective for general use; excellent coagulation capabilities. | Significant lateral thermal spread to adjacent tissues; high risk of collateral damage. |
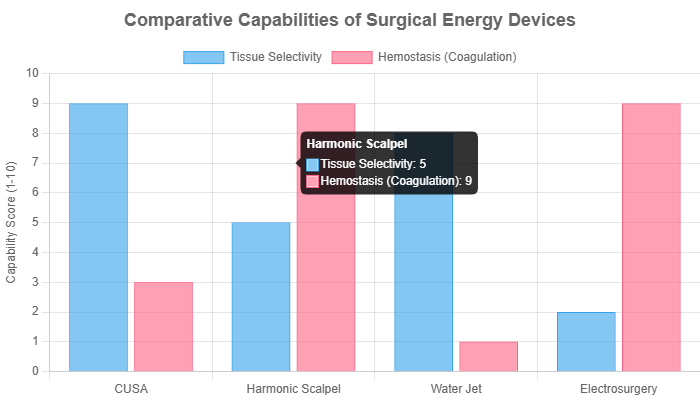
While the CUSA machine offers unmatched tissue selectivity, the Harmonic Scalpel combines cutting and coagulation in one step.
The Future of Ultrasonic Surgery: What’s Next for CUSA Technology?
The CUSA machine has been a workhorse in surgery for over four decades, but innovation has not stood still. The future of ultrasonic surgery points towards smarter, more integrated, and even more precise systems.
- Integration with Robotics: A significant frontier is the combination of the CUSA handpiece’s precision with the stability, dexterity, and control of a robotic surgical platform. Integrating ultrasonic aspirators into robotic instruments could enhance minimally invasive procedures, allowing surgeons to perform complex resections through small incisions with greater accuracy (Piezoelectric transducer design for a robotic instrument).
- AI-Powered Tissue Recognition: Researchers are developing “intelligent” ultrasonic aspirators. These next-generation devices use advanced sensors to gather feedback from the tip-tissue interaction and employ AI algorithms to analyze this data in real-time. The goal is to automatically identify tissue types (e.g., tumor vs. nerve vs. blood vessel) and potentially adjust power settings on the fly to maximize safety and efficiency (Intelligent ultrasonic aspirator study).
- Miniaturization and Enhanced Ergonomics: As surgery trends towards ever-smaller incisions (keyhole and endoscopic surgery), there is a drive to create smaller, lighter, and more ergonomic handpieces. This will allow for finer control and better access in constrained anatomical spaces.
- Novel Transducer and Tip Designs: The fundamental physics are also being explored. Research into novel vibration patterns, such as elliptical vibrations, aims to improve fragmentation efficiency for particularly challenging tissue types like cartilage or highly fibrous tumors, expanding the range of applications for the technology (Proposal for a novel elliptical ultrasonic aspirator).
Common Questions & FAQs
Is the CUSA machine completely safe around nerves and blood vessels?
It is significantly safer than most other energy devices due to its inherent tissue-selective nature. However, its safety is highly technique-dependent. A surgeon’s skill is paramount. Direct, prolonged contact, excessive pressure, or improper use (e.g., insufficient irrigation leading to heat buildup) can still cause thermal or mechanical injury. As with any powerful surgical tool, careful and trained technique is essential to harness its benefits safely. Studies have shown that thermal effects are a real risk that must be managed (Operative field temperature study).
What is the learning curve for a surgeon to become proficient with CUSA?
There is a definite learning curve. Surgeons need dedicated training to develop a tactile feel for the device and to master the adjustment of its parameters (amplitude, suction, irrigation) for different tissue consistencies. This proficiency is typically gained through hands-on training labs using models (like bovine liver) and proctoring by experienced senior surgeons during actual cases (Hands-on exercises on bovine liver).
Can CUSA be used on hard tissue like bone?
Yes, but this requires specialized systems. While standard CUSA tips are for soft tissue, specific ultrasonic surgical systems and dedicated tips (like the Misonix BoneScalpel or specialized tips for the CUSA Clarity) are designed for osteotomies (cutting bone). They use the same ultrasonic principle to precisely remove bone with minimal damage to nearby soft tissues like nerves or dura mater, which is a major advantage over traditional drills and saws that can cause significant vibration and thermal injury.
Is CUSA technology cost-effective?
This is a complex question. The initial capital investment for the console and the recurring cost of single-use disposables (tubing, tips) are significant. However, a strong argument for its cost-effectiveness can be made by looking at the total cost of care. By enabling more complete tumor resections, reducing blood loss (and the need for costly transfusions), and lowering the rate of complications, the CUSA machine can lead to shorter hospital stays and fewer re-operations, potentially offsetting its high upfront cost (Use in pediatric surgery and cost considerations).
Conclusion: The Enduring Impact of CUSA on Surgical Precision
The Cavitron Ultrasonic Surgical Aspirator is more than just a piece of equipment; it is a testament to how a deep understanding of physics can be translated into a tool that fundamentally changes surgical possibilities. For over forty years, it has empowered surgeons to operate with a level of finesse and safety that was once unimaginable.
Its value can be distilled into three core pillars:
- Precision: Its unparalleled ability to selectively fragment and remove diseased tissue while preserving the integrity of vital, healthy structures remains its defining characteristic.
- Efficiency: The elegant combination of tissue fragmentation, constant irrigation, and immediate aspiration into a single instrument streamlines complex procedures and maintains a clear, controllable surgical field.
- Safety: When wielded by a trained surgeon, the CUSA machine can significantly reduce collateral damage compared to thermal devices, directly enhancing patient safety and improving postoperative outcomes.
As technology continues to evolve with the integration of AI, robotics, and novel engineering, the principles pioneered by the CUSA will continue to form the foundation of the next generation of intelligent surgical tools.